Key Takeaways
- Gastro health goes far beyond digestion, acting as a central hub for your overall immunity and mental state.
- A balanced gut microbiome can significantly reduce the risk of chronic conditions like diabetes and heart disease.
- Approximately 70% of your immune system resides in your digestive tract, making gut care essential for fighting infections.
- Dietary choices rich in fiber and fermented foods directly support the beneficial bacteria needed for disease prevention.
- Stress and sleep patterns play a critical role in maintaining the delicate balance of your digestive ecosystem.
Did you know that your stomach might actually be the most important organ when it comes to staying healthy? We often focus on our hearts, our lungs, or our brains, but the lining of your digestive tract is where a massive battle for your health takes place every single day. If you have ever wondered why some people stay sick more often than others despite eating well, the answer often lies in their gut. In 2026, medical science has moved past the idea that digestion is just about breaking down food. It is now clear that Gastro Health is the comprehensive state of your digestive system's function, including the balance of bacteria, enzyme production, and mucosal integrity. This system acts as a gatekeeper, deciding what stays in your body and what gets flushed out.
When we talk about preventing disease, we usually think of vaccines or avoiding germs. However, the internal environment of your body is just as critical. A healthy gut acts as a shield, preventing harmful substances from entering your bloodstream. When that shield breaks down, often called "leaky gut," it can trigger inflammation that spreads throughout the body. This systemic inflammation is the root cause of many modern ailments, from autoimmune disorders to metabolic syndrome. Understanding how your digestive tract influences your entire physiology is the first step toward taking control of your long-term wellness.
The Immune Connection You Cannot Ignore
Most people assume the immune system lives in the lymph nodes or the spleen. The reality is much more surprising. About 70% of your immune tissue is located in the gut-associated lymphoid tissue (GALT). This means that every time you eat, you are interacting with your immune system directly. If your digestive health is compromised, your immune response becomes either too weak or too aggressive.
Think of your gut lining like a security fence. It allows nutrients to pass through while keeping bacteria and toxins out. When you consume processed foods high in sugar and unhealthy fats, this fence starts to develop holes. This condition, often referred to as increased intestinal permeability, allows undigested food particles and bacteria to leak into the bloodstream. Your immune system sees these particles as invaders and attacks them. This constant state of alert creates chronic inflammation. Over time, this inflammation can damage blood vessels and organs, paving the way for serious diseases.
Research published in recent years highlights the link between gut dysbiosis and autoimmune conditions. Dysbiosis is simply an imbalance of good and bad bacteria. When the bad bacteria take over, they produce toxins that irritate the gut lining. This irritation signals the immune system to attack the body's own tissues. By maintaining a healthy balance of bacteria, you reduce the likelihood of your immune system turning against you.
How the Gut Influences Chronic Disease
It is not just about catching a cold. The state of your digestive system has a profound impact on long-term conditions that develop over decades. Take type 2 diabetes, for example. Studies suggest that the composition of gut bacteria influences how your body processes glucose. Certain strains of bacteria help regulate blood sugar levels, while others can promote insulin resistance. If your gut flora is dominated by the wrong types of microbes, your body struggles to manage energy, increasing the risk of developing diabetes.
Heart disease is another major concern linked to digestive health. Some gut bacteria metabolize nutrients like choline and carnitine, which are found in red meat and eggs, into a substance called TMAO. High levels of TMAO in the blood are associated with an increased risk of heart attack and stroke. Interestingly, people with a diverse microbiome tend to produce less of this harmful compound. This means that simply changing the environment inside your gut can alter your cardiovascular risk profile without necessarily changing your diet entirely, though diet is the primary lever.
Even cancer risk is tied to the gut. Chronic inflammation is a known driver of cancer cell growth. Since the gut is a primary source of inflammation, keeping it calm and balanced is a form of cancer prevention. Specific bacteria, such as Lactobacillus and Bifidobacterium, have been shown to produce metabolites that protect the lining of the colon, potentially lowering the risk of colorectal cancer.
| Disease Category | Gut Mechanism | Prevention Strategy |
|---|---|---|
| Autoimmune Disorders | Intestinal permeability triggers immune attack | Reduce processed foods, increase fiber |
| Cardiovascular Disease | Bacteria produce TMAO from nutrients | Consume polyphenol-rich foods |
| Type 2 Diabetes | Microbiome affects insulin sensitivity | Prebiotics and fermented foods |
| Colorectal Cancer | Chronic inflammation damages cells | High fiber intake, limit red meat |
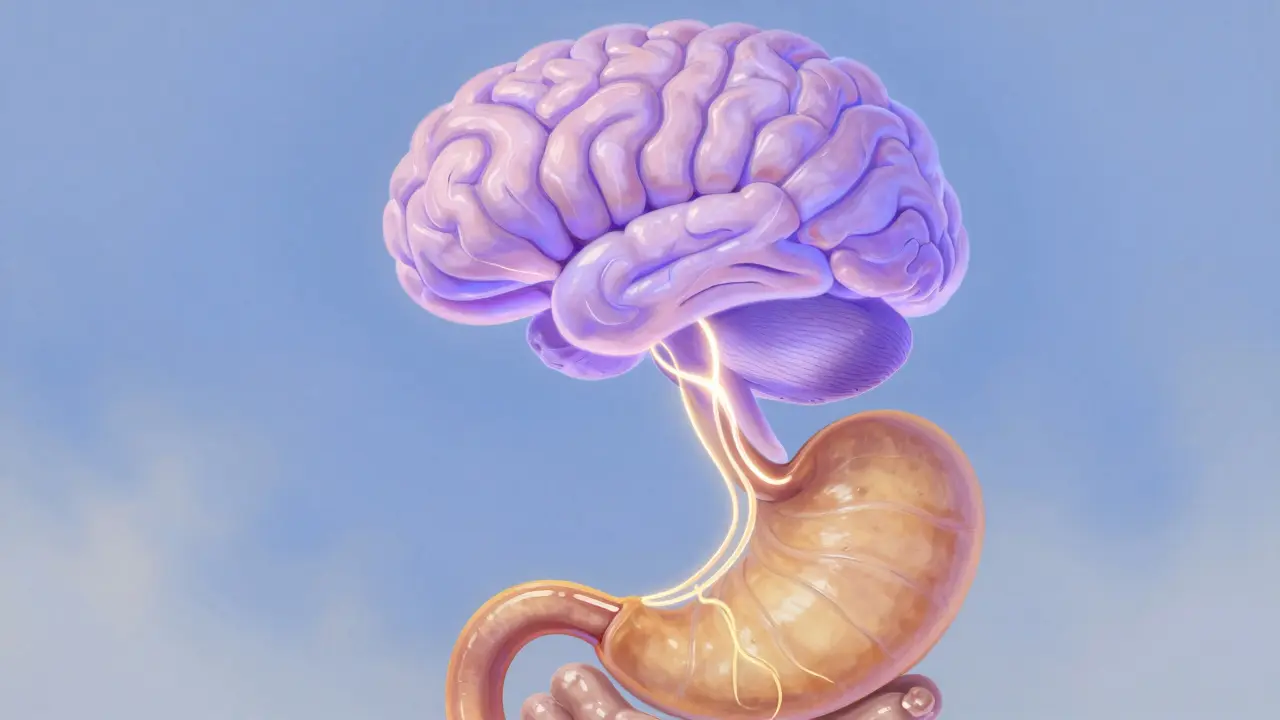
The Gut-Brain Axis and Mental Wellness
You might have heard the phrase "gut feeling" before. In 2026, we know this is scientifically accurate. The gut and the brain are connected by the vagus nerve, creating a two-way communication highway known as the gut-brain axis. This connection means your digestive health directly impacts your mood, stress levels, and cognitive function. About 90% of your body's serotonin, the chemical that makes you feel happy and calm, is produced in the gut, not the brain.
When your gut is inflamed or your bacteria are imbalanced, serotonin production drops. This can lead to anxiety, depression, and brain fog. Conversely, high stress levels send signals down the vagus nerve that disrupt digestion, slowing down movement and altering bacteria growth. It is a vicious cycle. To prevent mental health decline, you must treat your gut as part of your neurological system. Ignoring digestive symptoms like bloating or irregularity can eventually manifest as emotional instability.
This relationship also explains why stress often causes stomach upset. When you are under pressure, your body diverts blood away from digestion to your muscles. Over time, this lack of blood flow weakens the gut lining and reduces enzyme production. Managing stress is not just a mental health tip; it is a digestive health necessity. Techniques like deep breathing or mindfulness can physically change the pH and motility of your digestive tract.
Nutrition as Medicine for Prevention
If you want to use food to prevent disease, you need to feed the right bacteria. Not all healthy foods are created equal when it comes to the gut. The most critical nutrient for your microbiome is fiber. Fiber acts as a prebiotic, which means it is food for your beneficial bacteria. When these bacteria ferment fiber, they produce short-chain fatty acids like butyrate. Butyrate is the primary fuel source for the cells lining your colon, keeping them strong and preventing leaks.
Most people do not eat enough fiber. The average intake is far below the recommended 30 grams per day. You can increase this by adding beans, lentils, oats, and vegetables to every meal. However, it is not just about the quantity. Diversity is key. Eating a variety of plant foods ensures that different species of bacteria thrive. If you only eat the same five vegetables, you only feed the same five bacteria.
Fermented foods are another powerful tool. These foods contain live cultures of bacteria that can colonize your gut temporarily or permanently. Examples include yogurt, kefir, sauerkraut, kimchi, and miso. These foods introduce beneficial strains like Lactobacillus and Bifidobacterium directly into your system. In 2026, probiotic supplements are also widely available, but getting bacteria from whole foods is generally preferred because they come with other nutrients that support absorption.
It is equally important to know what to avoid. Ultra-processed foods often contain emulsifiers and artificial sweeteners that can strip away the protective mucus layer of your gut. This layer is your first line of defense. When it is damaged, bacteria can touch the gut wall directly, triggering inflammation. Cutting back on packaged snacks and sugary drinks is one of the fastest ways to lower your risk of digestive-related diseases.

Lifestyle Factors That Shape Your Gut
Diet is only half the equation. How you live your life matters just as much. Sleep is a major factor. During sleep, your body repairs the lining of your digestive tract. If you are chronically sleep-deprived, this repair process is interrupted. Studies show that people who sleep less than six hours a night have a less diverse microbiome compared to those who get seven to eight hours. Poor sleep also increases cravings for high-sugar foods, which further damages the gut.
Physical activity also plays a role. Exercise increases the diversity of gut bacteria. Even moderate walking can improve gut motility, preventing constipation and allowing waste to move through the system efficiently. However, excessive intense exercise without proper recovery can sometimes increase intestinal permeability, so balance is important.
Medications can also impact your gut health. Antibiotics are life-saving, but they wipe out both good and bad bacteria. If you must take antibiotics, it is crucial to replenish your microbiome afterward with probiotics and prebiotic foods. Even common painkillers like NSAIDs can irritate the stomach lining if taken frequently. Always discuss the long-term impact of medications with your healthcare provider.
Recognizing Warning Signs Early
Prevention works best when you catch problems early. Your body sends signals when your gut health is declining. Common signs include persistent bloating, frequent gas, irregular bowel movements, and food intolerances that develop suddenly. If you find yourself needing laxatives or antacids regularly, your system is struggling to function naturally.
Other signs might seem unrelated to digestion. Skin issues like eczema or acne, unexplained fatigue, and brain fog can all be rooted in the gut. If you experience these symptoms alongside digestive issues, it is worth investigating your gastro health. Blood tests can check for inflammation markers, and stool tests can analyze your microbiome composition. These tools provide a snapshot of your internal environment and help tailor a prevention plan.
Do not wait until you develop a chronic condition to take action. The gut has a remarkable ability to heal itself when given the right support. By prioritizing your digestive health today, you are investing in a future with fewer illnesses and more energy. It is not about perfection; it is about consistency. Small changes in what you eat and how you live can create a resilient system that protects you for years to come.
How long does it take to improve gastro health?
Improvements can often be felt within a few weeks of dietary changes, such as increasing fiber intake. However, fully restoring the microbiome balance and healing the gut lining may take several months to a year, depending on the severity of the imbalance.
Are probiotic supplements necessary for disease prevention?
They can be helpful, especially after antibiotic use, but they are not strictly necessary if you consume a diet rich in fermented foods and diverse plant fibers. Whole foods provide a broader range of nutrients and bacteria.
Can stress really cause digestive diseases?
Yes. Chronic stress alters gut motility and increases inflammation, which can lead to conditions like irritable bowel syndrome (IBS) and worsen inflammatory bowel disease (IBD). Stress management is a key part of gut care.
What foods should I avoid for better gut health?
Limit ultra-processed foods, added sugars, artificial sweeteners, and excessive alcohol. These substances can damage the gut lining and promote the growth of harmful bacteria.
Is there a specific test to check my gut health?
Yes, stool analysis tests can identify bacterial imbalances, inflammation markers, and digestion issues. Blood tests can also check for systemic inflammation and nutrient deficiencies related to absorption.
Taking care of your gut is one of the most effective ways to prevent disease in the long run. It is a proactive approach that empowers you to manage your health rather than just reacting to symptoms. By understanding the connection between your digestion and your overall wellness, you can make choices that protect your body from the inside out.